
ABSTRACT: "Bruxism" historically has been casually defined as "the clenching and/or grinding of the teeth". Since there can be no teeth grinding without the jaws first being clenched, a re-definition of bruxism is presented: Intense jaw-clenching, with or without forcible excursive movement, where the intensity of jaw-clenching dictates the severity of teeth-grinding. Traditional inter-occlusal splint methods of treating bruxism have been unpredictable because of their specific design to address grinding, when it is the degree of intensity of clenching which dictates severity of symptoms. A new device which suppresses clenching intensity by exploiting the nociceptive trigeminal inhibition reflex, is presented.
Individuals with a far less than ideal jaw relationship and/or occlusal scheme may be completely asymptomatic, while others who have ideal jaw relationships and occlusal schemes chronically suffer from debilitating headaches, face and jaw pain. Etiological research continues to show that essentially, it doesn't matter what a person has, or where it is...what matters is, what one does with what one has.(1)
Dentistry typically acknowledges that the activity responsible for these symptoms is bruxism. However, the current standard treatment for bruxism, i.e., a splint or nightguard, may not be entirely effective at resolving the patient's symptoms. The problem lies not in dentistry's mis-treatment, but of its mis-conception of the diagnosis, i.e., bruxism. This lack of understanding of the true nature of bruxism has resulted in the current standard of care for chronic TMD: management of symptoms(1,2,3).
Dentistry has stipulated that treatment with an inter-occlusal splint will result in one of three scenarios: the patient may improve; remain unchanged; or get worse(4,5). The reality is, treatment outcome using an traditional occlusal splint alone for patients with significant myofascial pain is no better than placebo(6). When treating TMD surgically, those patients with uncontrolled nocturnal bruxism are considered to have a poor prognosis(7). After elective orthognathic surgery, some procedures fail due to previously un-acknowledged, but suddenly destructive, bruxism. A patient cannot be informed of the risk of the potential adverse outcome if the provider himself doesn't fully understand the true nature of bruxism.
To gain an upper hand on bruxism, a better understanding of the term and therefore, the condition itself, is necessary. Bruxism is not a condition of the teeth. Teeth don't cause an activity, but are merely being affected by an activity(8). Dentistry is essentially the art and science of how healthy teeth occlude with each other. Dentistry reflexively treats most every condition it is presented with by addressing the health of the teeth, and their scheme of occlusion(9). However, bruxism is an act which results in the occluding of teeth, specifically, the intensity of occluding...which then results in a particular scheme of occlusion.
Bruxism is a function of clenching. The intensity of clenching dictates the severity of grinding. There is no teeth grinding unless the jaws are first clenched together. The jaws must be clenched together intensely enough to provide adequate resistance to lateral pterygoid activity, which then "grinds" the teeth in excursive movement. As the intensity of temporalis contraction (clenching) increases, resistance to mandibular lateral movement is increased, thereby increasing the efforts of the lateral pterygoids and strain on the TMJs. Therefore, as the intensity of clenching increases, the ability to move the mandible laterally (grinding) decreases. Ultimately, the most intense clenching would prevent any grinding of the teeth at all . With this observation, the appropriate definition of bruxism becomes apparent: "Intense jaw-clenching, with or without forcible excursive movement". The patient who presents with severely worn teeth, obviously a result of vigorous grinding, may have no symptoms to report, because they never exert adequate static clenching intensity to become symptomatic. Another with no indication of occlusal wear, but who complains of severe headaches and neck pain, but without TMD signs or symptoms, clenches intensely in centric position. Only by recognizing bruxism as a function of clenching can these patients be accurately diagnosed.
In a recent study of chronic tension-type headache patients without TMD, temporalis contraction (clenching) during sleep was shown to be, on average, fourteen times more intense than in asymptomatic control subjects(10). Clenching in centric position maintains a stabilized TMJ environment. However, the typical patient with chronic TMD (headaches, face and jaw pain, tooth wear) will forcibly grind their teeth to an excursive position, and then clench in that position ("grinding to a clench"), placing severe and often damaging strain on the TMJ(s)(11). There exists a dynamic relationship between the temporalis' and lateral pterygoids, from which signs and/or symptoms may result. The intensity of the temporalis activity combined with the degree of lateral pterygoid activity (if any), dictates the presentation of headache, TMD, or tooth wear.
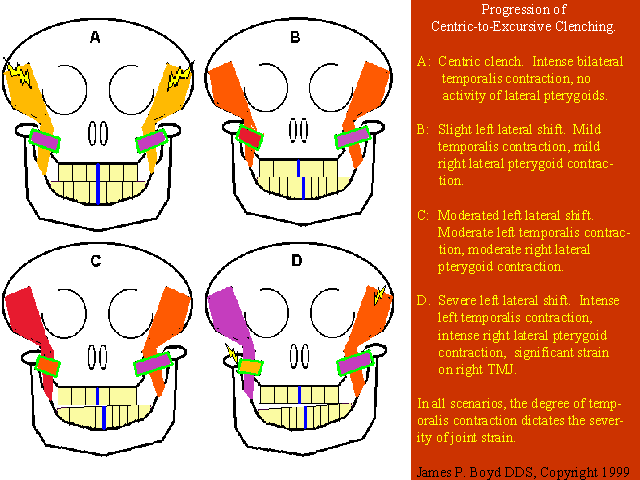
Ultimately, in order to treat and prevent bruxism, clenching intensity must be suppressed. Unfortunately, the traditional inter-occlusal splint, while decreasing resistance to lateral movement thereby relieving lateral pterygoid contraction and TMJ strain, provides improved resistance to the temporalis, allowing clenching to persist, or intensify(12).
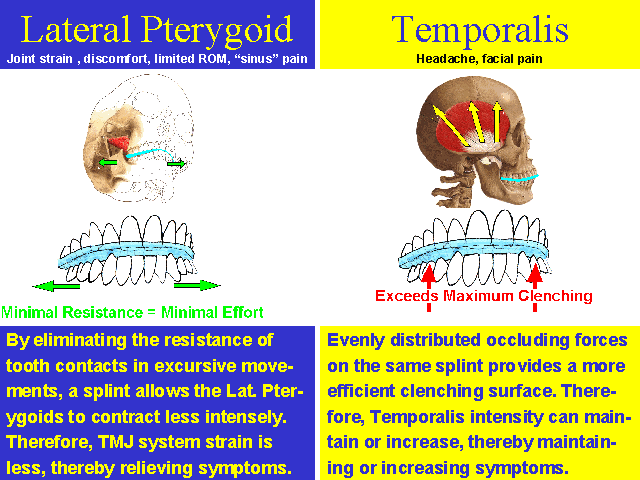
The success or failure of the traditional inter-occlusal splint is a function of the intensity of clenching. If clenching intensity persists or increases after using a splint, TMD treatment becomes TMD management.
Suppression of temporalis contraction (clenching) can be achieved by exploiting the nociceptive trigeminal inhibition reflex, also known as the jaw-opening-reflex (13,14,15). Direct pressure stimulation of the mandibular incisor's periodontal ligament activates a reflex loop which suppresses the temporalis' contraction intensity (conversely, anesthetization of the mandibular incisors PDL's allows clenching intensity to increase (16)). Historically, an anterior deprogrammer (such as a Lucia jig) or an anterior-point-stop (17), has been advocated to establish and record optimal condylar position (CR) and to suppress acute muscular symptoms on a short term basis. Each are effective in clenching suppression in centric positions. However, for the deprogramming jig, excursive movements of the mandible can allow for a mandibular canine to contact the device, allowing for ipsilateral near-maximal clenching (18) and joint strain while with the anterior-point-stop, protrusive movement of the mandible allows for posterior occlusion, allowing for near-maximal clenching. Clearly, all mandibular excursive positions, not just centric, must be considered when attempting to suppress temporalis clenching.
In response to this need, the NTI Clenching Suppression System (19) is now available. The key element to the NTI Clenching Suppression System is a patented pre-fabricated, easily retro-fitted anterior-point-stop device which suppresses clenching intensity in all excursive and protrusive movements.
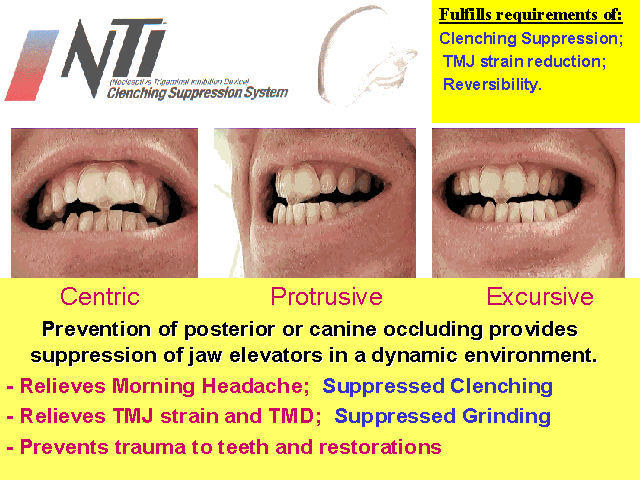
Used primarily during sleep, the NTI reduces voluntary clenching intensity to one-third of maximum (20). As described by Okesen (17), the NTI design allows for the best "musculoskeletally stable" (CR) position of the condyles, while suppressing hyperactive musculature. Additionally, by providing for no unilateral canine or posterior contacts, as can happen with a full-coverage splint due to contortion of the mandible in excursive movement (10), the NTI allows for the least amount of potential joint strain in any excursive or protrusive movements.
Two misconceptions of the NTI are not uncommon: posterior teeth may supra-erupt, and mandibular incisor(s) may intrude. Long term (five years or more) observations of nightly NTI use show that neither of which is the case (20). In order for a posterior tooth to supra-erupt, it must go unopposed for a considerable amount of time, long enough to allow bone growth at the apex (approximately six weeks is necessary for bone growth). Since it is impossible to masticate with the NTI in place, the daily stimulation of the posterior teeth prevent any adverse drifting or supra-eruption. As for incisal intrusion, a constant low-grade force must be maintained for a considerable amount of time before intrusion can occur. Even in the most extreme circumstances, clenching forces persist for only minutes, not nearly enough time to allow for permanent orthodontic movement or intrusion. Even in the case of the clinician's oversight, where the discluding element of the NTI (which provides the point stop) is not perpendicular to the long axis of the mandibular incisor (it should be), the patient will report a tenderness to the tooth immediately after the first night of use, and will resist wearing the device until addressed by the dentist, long before there is any orthodontic movement.
Although the NTI device itself does not cause any orthodontic movement, it can allow for repositioning of the mandible, due to its allowing for the most musculoskeletally stable condylar position. This is most noticeable in the patient whose condyles happen to seat more posteriorly and superiorly in the fossa as the patients symptoms resolve. As the condyle seats more posteriorly and superiorly, the mandible "pivots" typically at the last molars, with the anterior mandible rotating inferiorly and posteriorly. The patient's original degree of incisal overlap during CO dictates to what degree, if any, of resulting anterior open bite. Interestingly, when informed of the odds of this scenario occurring (less than 5%, and always accompanying the resolution of symptoms), patients are usually surprised if they percieve that the practitioner has placed the importance of their current jaw relationship above their chronic pain.
Unlike the traditional methods of splint fabrication and delivery (which typically require impressions, models, lab-fees, and the potential for numerous adjustment appointments), the NTI requires one simple chair-side procedure where the device can be fabricated and delivered in a 20-minute appointment. The relative small size of the NTI and its secure fit provides for excellent patient compliance, compared to the bulky and often irritating traditional splint. In clinical trials using the NTI, 83% of patients who had previously failed traditional splint therapy for chronic and/or acute TMD, had complete resolution or significant reduction of their symptoms within one month of nightly NTI use, and reported continued resolution at a one year follow-up.